FREE DOWNLOAD
Understanding Medicare Part D: “Preferred” vs “Contracted” Pharmacies
Getting Complaints from Residents & Families about Their Pharmacy Bills?
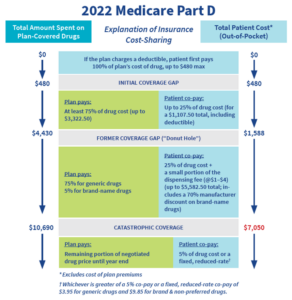
It’s that time of the year again…the dreaded Medicare Part D “Donut Hole,” where beneficiaries often face temporarily higher costs for prescription medications because of the coverage gap.
Although officially this gap was eliminated and costs should be lower than in the past, residents still may face increased medication costs and co-pays once they complete the initial coverage phase, having spent a total of $1,588 out of pocket. But there is still some good news.
- Using a long-term care pharmacy, residents actually reach better coverage levels faster by getting their out-of-pocket expenses to the annual maximum earlier. That’s because LTC pharmacies are usually assessed higher co-pays when insurance companies’ pharmacy benefit managers limit their “preferred” networks to retail and mail-order partners.
- Once a beneficiary’s out-of-pocket max is reached, co-pays are reduced drastically for the year’s remaining medication fills. Since the annual maximum is the same for all beneficiaries, the sooner it can be reached, the sooner co-pays decrease to only 5% of drug cost or a fixed amount of $4.15 for generics and $10.35 for branded and “non-preferred” drugs.
- While some argue that retail or mail-order pharmacies may be cheaper than LTC pharmacy, the fact is that Medicare D’s annual out-of-pocket liability for beneficiaries is capped to the same amount no matter what type of pharmacy is used. More importantly, LTC pharmacies provide many more dispensing, reimbursement, and clinical services specifically geared to improve outcomes in senior and residential care.
Complete the form to download the tip sheet.